- Newry: 028 308 33666
- Galgorm: 028 252 56093
- Omagh: 028 828 39678
Your Easy Guide To The Contraceptive Coil | Duality Health
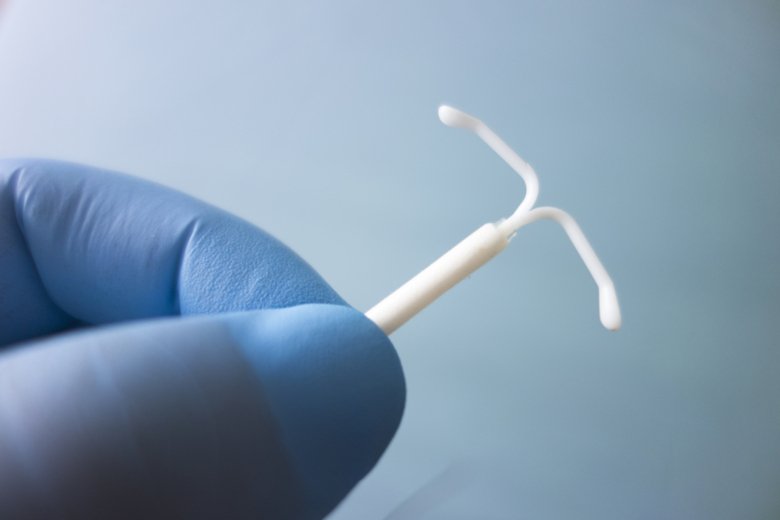
The coil is an effective form of contraception that prevents pregnancy and has minimal impact on your sex life. However, some women understandably find the prospect of coil insertion daunting and unfamiliar. This comprehensive guide contains the answer to all your questions and provides you with the relevant information you need to decide on whether the contraceptive coil is right for you.
The contraceptive coil is a T-shaped device that is placed inside your womb to prevent you from getting pregnant. It has one or two thin threads that hang through your cervix into the top of your vagina – these threads cannot be felt and are not uncomfortable. The coil works by stopping the sperm and egg from surviving in the womb or fallopian tubes, in addition to preventing fertilised eggs from implanting in the womb.
There are two types of coil used in the UK, the IUD and the IUS:
An intrauterine device (IUD) works by stopping the sperm from fertilising the egg and preventing implantation. It releases copper, which alters the state of fluids in the womb and fallopian tube and stops sperm from surviving there. The copper coil will start working immediately after it is fitted, meaning it can also be used for emergency contraception, and will be effective from between 5-10 years.
Some people opt for an IUD due to the fact that it does not cause any hormonal side effects. While it will not change the regularity of your periods, some people may experience longer, heavier periods – however these are likely to settle over time.
The other type of contraceptive coil is the intrauterine system (IUS). These coils contain a hormone called progestogen. This thickens the mucus from your cervix, making it difficult for sperm to move through and reach an egg. It also thins the lining of the womb, so that a fertilised egg cannot implant. This form of contraception works effectively for between 3-6 years, which means you won’t have to worry about contraception every time you have sex. There are three common brands of IUS that you will encounter in the UK:
- Mirena
- Levosert
- Jaydess
The contraceptive coil offers many benefits that make it a top choice over condoms and oral contraception:
- The coil works for an extended period of time, meaning you won’t have to worry about contraception every time you have sex.
- It is a highly effective form of contraception, with a success rate of over 99%.
- The coil won’t interrupt sex and is a hassle-free option.
- Your fertility will return to normal once the coil is removed.
- IUDs do not contain hormones, meaning you’re less likely to experience certain side effects that may be caused by contraception such as the oral pill.
- The hormonal-containing coil (IUS) can be used to help alleviate the symptoms of heavy or painful periods – they may stop completely after the first year of use.
- It can be used safely if you’re breastfeeding.
Most forms of modern contraception carry certain risks and side effects. This means it’s best to know all the facts before deciding on a contraception choice. These are the most common risks and side effects associated with the coil:
Within the first 3-6 months of coil insertion, it is common to experience irregular, prolonged or frequent bleeding. It’s important to remember that these bleeding patterns should improve with time. You may notice infrequent or no bleeding with the IUS (hormone containing coil).
With the IUS, some people may experience acne, breast tenderness, headaches or mood changes. These are likely to settle down over time.
When it comes to contraception, the coil is extremely effective. Only 5 in 1000 people will fall pregnant with this method, in comparison to oral contraceptive pills which fail 1 in 100 people.
An ectopic pregnancy occurs outside of the womb. In the unlikely event that a pregnancy does occur with a coil in place then up to 50% of these pregnancies may be ectopic. However, it is worth noting that you are much less likely to have an ectopic pregnancy while you’re using a coil than if you are not using any contraception at all.
In 1 in 20 people the coil can be pushed out by your uterus, or it can become displaced. This isn’t common and is more likely to happen soon after the coil has been inserted – you may not even know that it has happened. Your doctor or nurse will teach you how to check the threads so you know the coil is in place.
When it comes to getting a coil fitted, there is a very small risk that the coil may go through (perforate) your uterus or cervix. This can happen in up to 2 in 1000 insertions. While you may experience pain, there are usually no other symptoms and the uterus or cervix will heal by itself. In the case of perforation, the coil may have to be removed by surgery.
There is a small risk of infection after having your coil fitted. The risk is highest in the first three weeks after having your coil fitted, but can occur anytime whilst the coil is in. Here are some symptoms you should look out for:
- Pain the doesn’t settle
- Pain during sex
- A change in/increased discharge
- Generally feeling unwell
While pelvic infections are rare, it is important that you seek medical attention if you’re experiencing any of these signs.
You may be advised to undergo checks for STIs (sexually transmitted infections) before a coil is fitted. Remember, the coil will not protect you against sexually transmitted infections. The best way to protect yourself is to use a condom with a new partner until you both have been tested.
Prior to coil insertion, you will likely have an initial consultation that will determine whether the coil is the right choice for you. Your doctor or nurse will answer any questions you may have. They will also ask you about your sexual and general health – in most cases, you will be offered a swab test to check for sexually transmitted infections (STIs) such as chlamydia and gonorrhoea. Remember, a coil cannot be fitted if there is a risk of pregnancy. Many sexual health practices will ask you to use a reliable form of contraception until after the coil is fitted or abstain from sexual intercourse from the first day of your period or for 3 weeks before the appointment date.
You will also be examined to check which way your womb is lying and to study the cervix. This will be similar to getting a smear test.
Having a coil fitted can be uncomfortable, and some women may find it painful. You might experience mild abdominal discomfort, similar to period pain, during the procedure. Taking a dose of your usual painkiller, such as paracetamol or ibuprofen, can help reduce this – you may also be offered a local anaesthetic injection.
Some patients can feel shaky after their appointment, so it might be a good idea to have someone available to take you home afterwards. Most women will require a check-up a few weeks afterwards to ensure everything is going smoothly.
If you’re interested in discreet contraceptive coil insertion or removal services, Duality Health Ltd can help. Our private coil fitting service is broken down into two appointments, so that we can ensure everything runs smoothly and safely. You will have a consultation first with one of our trained professionals to check that you are suitable for a contraceptive coil insertion. Your medical professional will go over a few things with you to put your mind at ease and answer any questions you may have. After your consultation, your second appointment will be your private coil fitting, where you can trust in the expertise and care of our trusted professionals. To find out more about our private GP services, please call 028 3083 3666 today.